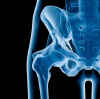
 Although doctors focus on bone density to diagnose osteoporosis and risk of bone fracture, the strength of bone is more complicated than that. The term bone quality is sometimes used to get at the resistance to breaks and overall strength. It is not quantified in any agreed-upon manner. One researcher called it "the geometric and material factors that contribute to fracture resistance."
Although doctors focus on bone density to diagnose osteoporosis and risk of bone fracture, the strength of bone is more complicated than that. The term bone quality is sometimes used to get at the resistance to breaks and overall strength. It is not quantified in any agreed-upon manner. One researcher called it "the geometric and material factors that contribute to fracture resistance."
Everything other than density that affects bone strength can be lumped into bone quality. Bone strength is a function of quantity of boney material (density) and quality.
Bone quality is affected by the architecture of the tissue at a microscopic level – meaning the patterns of bony and spongy material, shape of the bony structures, and position of collagen and osteoblasts and osteoclasts. Small fractures at this level affect bone quality, as does the length, density, and thickness of the collagen strands. The size and shape of the hydroxyapatite crystals influence how fast the minerals deposit and are reabsorbed to the bloodstream. The crystal morphology at a microscopic level is arguably part of bone quality.
And this stuff matters. Big picture: Bones affected by osteoporosis have low mineral mass and density and are affected by microarchitectural deterioration of the skeleton.
Tensile strength, elastic modulus, and compressive strength are metrics scientists and engineers use to describe material. Physiologist may use these terms to talk about bones, but as a practical matter these properties are not measured in the clinic with regard to diagnosis or treatment of bone diseases.
The statistical T score is (or should be) a surrogate marker for decline in bone quality and lowering of the bone’s Young’s Modulus. It is well known that the T-score has limits and is not a perfect proxy for bone strength.
Bone strength does not correlate directly with bone density, but there is a relationship. It is not linear and it is not general across all people so it is not necessarily true that increasing your bones’ density increases their strength. Indeed one barb thrown against bisphosphonates is that they are better than hardening bone than strengthening bone.
Even two bones with the same density may have markedly different qualities and strength. Young bone is generally stronger than old bone, even at the same density. Different people in their 20s have different bone densities due to genetic differences. And maybe absolute density doesn’t matter as much as changes. It may be true that the risk for fracture is influenced more by changes in density over time than to absolute density. It would be ideal if each person had their densities recorded at age 25 or 30 and could refer to them later in life, but the health care system today does not support that.
 Contrary to what you might think, bones are not hard or brittle or lifeless. People might get the lifeless idea from seeing bones outside the body. Living bone is as alive as any other organ. It uses energy (calories), oxygen, and has blood vessels coursing through it.
Contrary to what you might think, bones are not hard or brittle or lifeless. People might get the lifeless idea from seeing bones outside the body. Living bone is as alive as any other organ. It uses energy (calories), oxygen, and has blood vessels coursing through it.
Imaging and diagnostic tools that can help get at the microarchitecture of bone but tying this to bone quality or bone density is not straightforward. In the future, computed tomography (CT scans) and high-resolution magnetic resonance imaging (MRI) scans and better mathematical models of bone physiology may allow doctors to elucidate quality without taking biopsies. This has to be worked out, however, and the norms and standards established so that the results of the tests can be translated to a risk of bone fracture and osteoporosis.
 DEXA scans are cheap and painless, which is why they are so widely used. But they are not reliable. Different machines can produce different readings, resulting in interpreted bone densities of up to 10%. Given that the standard deviations in bone densities are only about 10%, this is a huge potential factor in misclassifying people as having osteopenia, osteoporosis, or healthy bones. Further, if a patient has a DEXA scan two years in a row on two different machines, the results could suggest a rapid loss or gain in bone density, giving a misleading picture about the efficacy of treatment and state of skeletal health. To be accurate, the patient should be measured in the same DEXA scan every time, and that is not always feasible.
DEXA scans are cheap and painless, which is why they are so widely used. But they are not reliable. Different machines can produce different readings, resulting in interpreted bone densities of up to 10%. Given that the standard deviations in bone densities are only about 10%, this is a huge potential factor in misclassifying people as having osteopenia, osteoporosis, or healthy bones. Further, if a patient has a DEXA scan two years in a row on two different machines, the results could suggest a rapid loss or gain in bone density, giving a misleading picture about the efficacy of treatment and state of skeletal health. To be accurate, the patient should be measured in the same DEXA scan every time, and that is not always feasible.
The range of bone densities used to establish T-scores is a reference set taken by someone. Who? The American Medical Association? The International Society for Clinical Densitometry? We can’t find the answer to that question. It might be the manufacturers of DEXA machines who set the references.
In any case, the reference set is said to be the densities of bones (hip, spine, wrist, etc.) for people at age 30. (It used to be age 25, but now 30 is more often mentioned.) There are separate reference sets for men and women. There do not appear to be separate reference sets based on race or area of the world where the patient resides, although some people feel these should be factored into the T-score.
The International Society for Clinical Densitometry claims scans are a better predictor of bone fractures than hypertension is of strokes or high cholesterol is of heart attacks. Of course the ISCD is a professional organization of technologists that do these scans, which may bias their statements.
A recent study in Australia of patients who take bisphosphonates shows that although the drugs work, regular bone density scans in the years following initiation of treatment are not cost effective. This is due to the inaccuracy of the scans and the low variability in response to the medicine.
The International Society for Clinical Densitometry responded that the Australian authors did not account for all possible biases in the clinical studies they considered. The criticism sounds rather weak to us.
